Press Release, as provided by Congenital Hyperinsulinism International:
Hyperinsulinism Awareness Day Will Be Observed Saturday, June 7
For Immediate Release: May 12, 2025
Glen Ridge, NJ – Congenital Hyperinsulinism International (CHI) is excited to announce that June 7, 2025 will be Hyperinsulinism Awareness Day. Congenital hyperinsulinism (HI) is the most frequent cause of severe, persistent hypoglycemia (low blood sugar) in newborns.
“Hyperinsulinism is something everyone should know about because the worst consequences of the condition are all preventable with timely recognition and management,” says Julie Raskin, CEO of CHI. “CHI raises global awareness of the condition and offers vital support to those affected and their families. No one should have to face HI alone.”
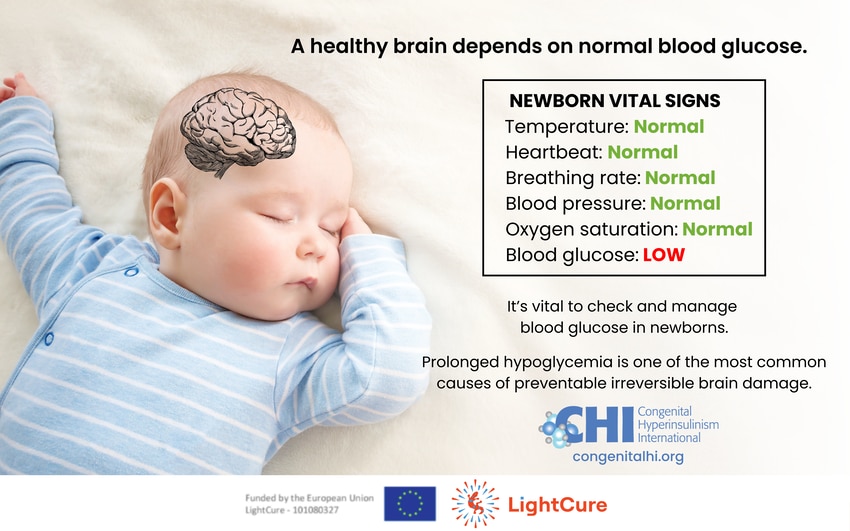
Untreated or improperly treated hypoglycemia can be dangerous because the brain relies on glucose as its primary source of energy. Without enough glucose, permanent brain damage can occur, potentially impacting a child’s development. The risk of brain damage is higher if HI is not diagnosed and treated quickly or if treatment does not work well at preventing ongoing hypoglycemia. However, with the right treatment, hypoglycemia can be managed, and brain damage can be avoided. Treatment options for people with HI are actively evolving through on-going clinical trials.
In most countries, Persistent HI has an incidence of up to 1:28,000 births. Some forms of HI are linked to a genetic defect and can persist throughout life; others will resolve more quickly and are considered transient. Transient cases are far more common, occurring as frequently as 1 in 1,200 births. Brain damage is a risk in both cases. CHI hopes that HI Awareness Day will create a broader knowledge of the condition, as well as better understanding of the need for prompt diagnosis and management by established protocols.
“In babies with HI, the pancreas secretes insulin in an uncontrolled way, even when blood glucose levels are low. These babies present at birth with severe hypoglycemia that can lead to irreversible brain damage. Therefore, recognizing the condition and treating it is of the greatest urgency,” says Diva De Leon, Director of the Hyperinsulinism Center and Chief of the Division of Endocrinology at the Children’s Hospital of Philadelphia. “In hospital maternity wards and pediatricians’ offices, glucose is a vital sign that must not be ignored.”
###
About CHI
CHI, a nonprofit 501(c)3, is a global organization dedicated to supporting children and adults born with HI. CHI is a leading source of funding for research for better treatments and cures, and the foremost advocate for increased awareness and better medical protocols for HI in order to reduce preventable brain damage and death from prolonged hypoglycemia.
Contact
For more information, contact Lily Barnett, CHI Communications Associate, at lbarnett@congenitalhi.org or 973-544-8372.